May 19 2016
Medical Taylorism, Lean, and Toyota | P.Hartzband and J. Groopman | New England Journal of Medicine
Seen today in the New England Journal of Medicine, under the signature of Harvard Medical School professors Pamela Hartzband and Jerome Groopman:
“The TPS is a set of principles designed for the manufacture of inanimate objects in a factory. We accurately depict two essential elements of this system that are directly derived from Taylorism: standardization and time efficiency. In his classic study of the application of Toyota principles to the manufacture of cars in the United States, Paul Adler describes how ‘Each job was analyzed down to its constituent gestures, and the sequence of movements was refined and optimized for maximum performance. Every task was planned in great detail, and each worker was expected to perform that task in the prescribed manner.’ Adler refers to ‘the intelligent interpretation and application of Taylor’s time and motion studies’ as key to its success. He states, ‘The reference to Taylor may be jarring, but it fits.’
[…] Other medical professionals who, like us, have experienced the toxic effects of obsessive standardization and time efficiency in the care of patients have expressed concerns similar to ours. In an era of accountability, we believe that those who advocate the application of Lean principles to medical care must take responsibility for the unintended consequences resulting from these elements shared by Taylorism and Toyota practices.”
The authors base their claim that the Toyota Production System (TPS) is “derived from Taylorism” from the writings of Paul Adler, a business school professor at USC who has written many papers over the past 40 years, a few of which touched on TPS and NUMMI, the first plant to apply this system in the US and now operated by Tesla. I met Paul Adler at Stanford in the late 1980s, and found his insights on NUMMI quite valuable. It was also clear to me that Paul Adler was not an engineer, that TPS, to him was one interest out of many, and that his knowledge of the subject was only at the business school level, as reflected, for example in an expression like “Taylor’s time and motion studies.” Taylor did time studies; Frank and Lilian Gilbreth, motion studies with, as stated in other posts, very different objectives.
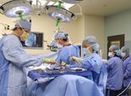
This distinction, perhaps too subtle for business schools, is of paramount importance to anyone who wants to understand TPS, which owes much more to the Gilbreth’s work than to Taylor’s. Taylor wanted to prevent workers from slacking off; the Gilbreths, to observe the way work was being done and make it easier. And the medical profession has a good reason to remember Frank and Lilian Gilbreth: the way operating rooms function today is based on the analysis and recommendations they made 100 years ago.


Jun 8 2016
This Doctor is Upset, But It Doesn’t Really Sound Like Lean | Mark Graban | leanblog.org
“[…] it’s a first-hand story and an opinion piece. […] Dr. Cotton describes the poor treatment he’s received from a 40-something internal “Lean consultant” named Dean. […] Dr. Cotton describes a typically hectic E.D. scene where he’s “six patients behind” and he’s spent some time talking to a patient’s mom in an attempt to comfort her and explain the situation… a perfectly human and caring response. Then, Dr. Cotton describes an interaction that I’d hope would never happen[…]: ‘And that’s when Dean confronted me. ‘He wasn’t your patient! You are six patients behind!” Dean was the hospital’s MBA consultant for LEAN management.”
Sourced through Scoop.it from:www
Michel Baudin‘s comments:
I think what happened to Dr. Cotton is primarily the result of 25 years of Lean bandwagon jumping. Ever since the name was coined, all sorts of consultants and gurus have rebranded their offerings as “Lean,” misleading their audiences and living off the reputation of the Toyota Production System.
Given the absence of consensus on a Lean body of knowledge or control on the appellation, this was inevitable. But this process has besmirched the “Lean” label, and I am not sure it is salvageable.
Dr. Cotton seems to have it in for MBAs, which Mark may think unfair because he has one. Mark’s saving grace, however, is that he is also a mechanical engineer.
See on Scoop it
Share this:
Like this:
By Michel Baudin • Blog clippings 3 • Tags: Lean Health Care, Lean Hospitals, MBA